- Blog
- Overcooked 2 pc
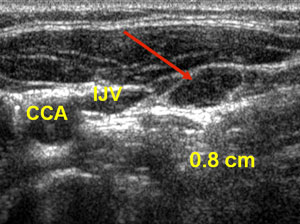
- Early stage cancer lymph nodes in neck
- Activation code for tune sweeper
- Unity networkview depricated
- Free math calculator
- Popeyes sweetie crossword clue
- Airmail stephen glass
- 7 days to die console commands seed
- International cricket captain 2016 tpsi
- Android barcode scanner
- Euphoria nude
- Pretty good solitaire free online
- Ableton live lite serial
- Android sm64 color code generator
- Chess plus score open

This was conducted by the Efficiency and Safety Evaluating Committee who were satisfied by the results of the interim analysis. A stopping rule was built into the Protocol (online only) after an interim analysis that was performed when half of the patients were followed up in 6 months.
#Early stage cancer lymph nodes in neck trial#
This trial was registered in the UMIN Clinical Trials Registry (UMIN000006510) in November 2011. Written informed consent was obtained from all participants. The study was initiated after ethics committee's approval from each institution (September 2011) and performed under the Safety and Efficacy Evaluation Committee's oversight. The retrospective and phase II studies 5, 6 have been performed before the phase III study. This multicenter, randomized, controlled phase III trial involving 16 Japanese centers, evaluating SLNB-navigated ND's noninferiority (SLNB group) compared with elective ND (ND group) in tumor category (T) T1-T2N0 OCSCC, was designed by the Head and Neck Cancer Micrometastasis Research Group and funded by the Japanese Ministry of Health, Labour, and Welfare. We conducted a randomized, multicenter, noninferiority, phase III trial, comparing SLNB-navigated ND with elective ND in early-stage OCSCC, and studied the postoperative survival rate, safety, and neck function.

Since reports of SLNB for OCSCC are limited and detection methods vary, a prospective multi-institutional study with numerous cases constituting unified methodologies is essential for verifying the validity of SLNB. 4 Appropriate ND might be achieved if SLNB is used for treating OCSCC. SLNB has been established as the method for staging patients with clinically N0 breast cancer and cutaneous melanoma and provides useful information of the nodal status. Performing SLN biopsy appropriately requires the expertise of a skilled head and neck surgeon, along with the collaborative efforts of a radiologist and a pathologist for pre-, post-, and intraoperative diagnoses. In this study, we compared SLN-navigated neck dissection versus elective neck dissection in early OCSCC and showed that SLN-navigated neck dissection was noninferior to elective neck dissection in terms of the survival rate, and superior in terms of neck functionality. There is insufficient evidence supporting a single strategy. However, avoiding unnecessary neck dissection prevents risks and complications, thus reducing surgical intervention and prolonged hospitalization.
A large-scale randomized controlled trial reported the superiority of elective neck dissection over observation. What is the best surgical technique for managing node-negative neck in oral cavity squamous cell carcinoma (OCSCC)? Potential strategies for managing patients with early OCSCC include observation, elective neck dissection, and sentinel lymph node (SLN) biopsy.

3National Cancer Center Hospital, Tokyo, JapanĤInternational University of Health and Welfare, Mita Hospital, Tokyo, JapanĦKyoto Prefectural University of Medicine, Kyoto, JapanĨSaitama Medical University International Medical Center, Hidaka, JapanĩGraduate School of Medical Science, Kanazawa University, Kanazawa, Japanġ0Faculty of Medicine and Graduate School of Medicine, Hokkaido University, Sapporo, Japanġ1Gunma University School of Medicine, Maebashi, Japanġ2University of the Ryukyus Faculty of Medicine, Okinawa, Japanġ3National Defense Medical College, Tokorozawa, Japanġ4Fukushima Medical University, Fukushima, Japanġ5Kyorin University School of Medicine, Mitaka, Japanġ6National Cancer Center Hospital East, Kashiwa, Japanġ7Aichi Cancer Center Research Institute, Nagoya, Japanġ8Kouseikai General Clinic and Hospital, Kawagoe, Japan
